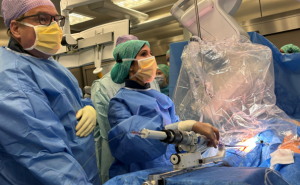
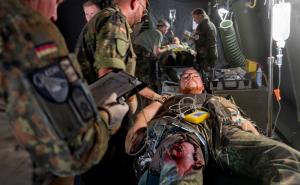
What’s new in U.S. Air Force Medicine
Das amerikanische Military Health System befindet sich derzeit in der umfangreichsten Reform der letzten 30 Jahre mit deutlichen Verschiebungen von Verantwortung zur Defense Health Agency, der Übertragung aller festen Behandlungseinrichtungen an die Defense Health Agency und einer zunehmenden Fokussierung der Sanitätsdienste der Teilstreitkräfte auf die ‘Medical Readiness’ des eigenen Personals und der ‘Readiness der Medical Forces’, also der sanitätsdienstlichen Elemente für den Einsatz (vgl. WM IV-2018) in den TSK. Diese Reform wirkt sich deutlich auf die Strukturen, Verantwortung und Schwerpunkte des Air Force Medical Service aus, den man bisher als einen umfassenden eigenständigen Sanitätsdienst betrachten musste. Im Interview umreißt Lt. Gen. Hogg, Surgeon General der Air Force, die Auswirkungen auf den Air Force Medical Service.
Ma’am, you became the 22nd Air Force Surgeon General in June 2018. How is it to be the first woman holding this position and also the first nurse to serve as the Air Force Surgeon General?
I am incredibly honored and humbled to have this position. I am a Women’s Health Nurse Practitioner by training and have practiced that the majority of my career. Even as I advanced in the ranks I was still able to practice to a more limited degree. I have been very supported by the members of the Air Force Medical Service. I also think that we have a great team in which to move the Air Force forward in today’s very challenging environment, filled with a lot of change that is currently going on in the U.S. Military Health System at large.How does the current Military Health System reform impact the Air Force Medical Service? What will be the major changes for Air Force medicine?
In the past the service medical departments had the responsibility of balancing delivering the benefit of health care to the beneficiaries and delivering readiness. Many times these were complementary, but also there were times where these were not complementary. The new transformation is going to give the delivery of the benefit of health care to the Defense Health Agency with the Services supporting the DHA. This gives a clear direction that medical readiness is the services‘ responsibility being supported by the DHA. I am going to take that and refocus our energy on paying attention to medical readiness as it relates to the medical readiness of my Airmen across the Air Force, and also on the medical readiness of my medics, by focusing on the training, the currency and competency required to keep my medics ready where they need to be at any given time should we need to do the mission.
What will the responsibilities of the Air Force Surgeon General look like in future and could you please give an example for readiness of the Airmen, please?
I don’t see the future of the Air Force Surgeon General changing a lot, except that it will become a little bit more single-minded in the sense that I will be focused on the medical readiness of the Airmen and the ready medic. The delivery of the health care to our Airmen and the beneficiaries will be something that I will collaborate with the Defense Health Agency in order to ensure we continue to provide safe, quality care either in our military treatment facilities or in the civilian network. My primary mission is to be the principal medical adviser to the Secretary of the Air Force und the Air Force Chief of Staff and to give them my best medical advice in how to support and enable the Air Force mission to be more effective. That mission and responsibility will stay the same. The way I am going to do that is reorganizing our structure by building a Field Operating Agency that will be strictly focused on readiness as it relates to education, training and competencies. And I will restructure the military treatment facilities to have an Operational Medical Readiness Squadron as a clinic where we have laser focus on the ‚mission capable‘ status of our Airmen. Our line officers are very in tuned to what their ‚mission capable‘ rate is of any given platform, aircraft or vehicle. But we have not done that well on the medical side and on the ‚human weapon system‘. I like to call it ‚human weapon system‘. We need to get better at maintaining that ‚human weapon system‘. We as medics are the maintainers of the ‚human weapon system‘. So this Operational Medical Readiness Squadron will focus strictly on active duty Airmen and we will ensure that when they become medically non-mission capable we are focused on making sure we take the necessary steps we need to provide the care needed, or get the referrals need to get that Airman back to full mission capability or we put her or him into the disability system if we won’t be able to get them back to being fully mission capable.What will the AF Medical Service’s focus be in future?
I have three goals for the Air Force Medical Service that we are working towards. One is full spectrum readiness, the other one is to develop joint leaders and the third is to proactively manage the Military Health System and the Air Force Medical System transformation. Under the full spectrum readiness the definition of an operator for the Air Force has changed over the years. We used to just identify flyers as operators in the Air Force, but we now know that our operators are much broader than just the pilot. We have security forces, we have ISR (Intelligence/Surveillance/Reconnaissance) forces, Remotely Piloted Aircraft pilots and so on. The plan is to bring a flight medicine like capability to all of our operators in this Operational Medical Readiness Squadron. So flight medicine will stay, because we will need that, but it will evolve and become much broader than that. So that we will then take care of all of our operators with a flight medicine like capability.
Will the Air Force Medical Service be impacted by reductions in staffing/personnel and how do you want to meet operational requirements?
Yes, we are reducing. Our analysis has shown what we need to do the operational mission and we currently have more active duty members than we actually need. We will reduce in number over the next several years to be more focused on operational medicine with the Defense Health Agency picking up the delivery of the benefit of health care. We will still have uniformed medics in military treatment facilities because they need to be there to maintain their currency and competency, but I believe that in the future you will either see more civilian medics delivering health care within the MTF or that the benefit of health care moves out of the military treatment facility and into the Tricare network or the surrounding market if there is capacity and capability to absorb that.
You had been stationed in Germany for three years during your career. How important are international collaborations for the Air Force Medical Service?
I think that the international collaboration, not only for the Air Force medicine, but for the Military Health System at large, so Army, Navy and Air Force, is incredibly important. We have the capacity and capability to really share lessons learned from each other where we don’t have to reinvent the wheel. The German Medical Service might have cracked a nut on a certain process or issue and sharing those between us makes us stronger. For me health is a universal language. We all want to have healthy service members because it’s more beneficial for the country or the globe at large. Sharing those health problems we have been successful at with other international partners is extremely important and we need to not lose that strength. In addition I think our ability to move around all over the globe in different countries and different cultures makes us as medics stronger in being able to understand some of the differences about health care and treatment and being more resilient and accepting some differences around the world. Medical is sometimes the easiest way to build relationships. As I said before, health as a universal language. We need not forget that and not to take for granted that medicine absolutely has a very significant place in building relationships with our partners.
Korrespondenzadresse des Autors:
Oberstarzt Dr. Kai Schlolau
[email protected]
Datum: 08.08.2019
Quelle: Wehrmedizin und Wehrpharmazie 2/2019