14. internationale Medizinische C-Schutz-Tagung 2013
(Abstracts Teil 1)
Read more about the abstracts of the 14. international CBRN-Defense
14. Internationale Medizinische
C-Schutz-Tagung
Am 24. und 15. April 2013 fand die 14. Internationale Medizinische C-Schutz-Tagung des Instituts für Pharmakologie und Toxikologie der Bundeswehr (InstPharmToxBw) unter der wissenschaftlichen Leitung von Oberstarzt Prof. Dr. Horst Thiermann mit dem Schwerpunktthema „Umsetzung experimenteller Forschungsergebnisse zur Verbesserung der Therapie bei Vergiftung durch chemische Kampfstoffe“ in den Tagungsräumen der Sanitätsakademie der Bundeswehr in München statt (Abb. 1).
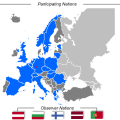
Mit über 200 Gästen aus 24 verschiedenen Nationen wohnten auch in diesem Jahr die weltweit führenden Experten auf dem Gebiet des Medizinischen C-Schutzes der Tagung als Teilnehmer und Referenten bei. Generalarzt Dr. Erika Franke eröffnete als Stellvertreterin des Amtschefs des Sanitätsamtes der Bundeswehr die Tagung (Abb. 2). Sie betonte dabei insbesondere die mobilen, hoch leistungsfähigen und in kritischer Situation lebensrettenden Diagnostika, die auf die Forschungs- und Entwicklungsarbeit am Institut für Pharmakologie und Toxikologie der Bundeswehr zurückgehen. In Vertretung für den Staatssekretär Gerhard Eck aus dem Bayerischen Staatsministerium des Inneren begrüßte Ministerialdirigent Alois Lachner die Tagungsteilnehmer und drückte die hohe Wertschätzung gegenüber dem InstPharmToxBw als leistungsfähigen Partner am Forschungsstandort Bayern aus.
Einleitende Vorträge von Referenten aus dem Bundesministerium der Verteidigung und dem Bundeswehrkrankenhaus Hamburg stellten den Kontext zu den Anforderungen der Bundeswehr und ihres Sanitätsdienstes im Einsatz her.
In den verschiedenen Sitzungen mit 26 Vorträgen und anhand von 44 Postern wurden der medizinische C-Schutz für den Einsatz, Aspekte der Lungentoxikologie und der Hautkampfstoffe, Therapieansätze bei Nervenkampfstoffvergiftungen sowie weitere experimentelle und klinische Aspekte bei Vergiftungen mit phosphororganischen Verbindungen beleuchtet und rege diskutiert.
Insbesondere die Entwicklung von alternativen Antidoten wie Bioscavengern und Rezeptormodulatoren stellt bei den noch bestehenden therapeutischen Lücken einen interessanten und vielversprechenden Ansatz dar, um die Versorgung der Soldaten unter C-Bedingungen weiter zu optimieren.
Ausgewählte Originalarbeiten werden in einem Sonderband von Chemico-Biological Interactions mit dem Titel “Fourteenth International Medical Chemical Defence Conference 2013: Translation of experimental research for improved treatment of chemical warfare agent poisoning” publiziert.
An Fragen des Medizinischen C-Schutzes Interessierte finden in dieser Ausgabe auf den folgenden Seiten und in einer der nächsten Ausgaben der Wehrmedizinischen Monatsschrift die Abstracts einzelner Vorträge und Poster. Letztere werden des weiteren in der „CHALLENGE – CBRN Medical Defense International“ abgedruckt.
Die 15. Medizinische C-Schutz-Tagung wird am 22. und 23. April 2015 in München stattfinden.
CBRN Threat – Conclusions for the conceptual design of CBRN Defence
Bosse, FB
Federal Ministry of Defence, Bonn, Germany
Nations’ security continues to be impaired by risk factors such as the destabilizing consequences of even distant crises and conflicts, international terrorism and the proliferation of weapons of mass destruction and their delivery vehicles. Non-governmental players, organized crime and asymmetric methods of using force pose further challenges for the Armed Forces in the conduct of its operations. The elements it is up against, some of which are militarily organized, while others fight asymmetrically, are attempting to compensate for their “conventional” inferiority in terms of force strength, equipment and training by applying „unconventional“ tactics, generally have access to all the weapons, ordnance, equipment and ammunition traded on the open world market or on black markets. It must be assumed that such forces will also be able to come into possession of nuclear, radiological, biological or chemical weapons or hazardous CBRN substances. In operations, force survivability is of utmost importance with respect to the threat or use of CBRN weapons or the release of hazardous CBRN substances, such actions being referred to here as „CBRN incidents“. Forces must therefore be able to conduct operations not only when there is a CBRN threat, but also in a CBRN environment. CBRN defence encompasses all the precautions and measures that can be taken to combat the effects of CBRN incidents across the mission spectrum both in the event of an CBRN threat and in an CBRN environment. In terms of function, CBRN defence is a support task, with preventive and reactive components in the corresponding capabilities. As a long-term and continuous process of adaptation to constantly changing conditions is required, the further conceptual development of CBRN defence will have to set objectives, signposts and principles for Armed Forces as a whole, within the scope of applicable laws. The objective is to adapt CBRN defence capabilities to the threats posed by CBRN weapons and hazardous CBRN substances, to the further development of legal parameters and to operational requirements. It is important for this development to be justifiable in economic terms, manageable in budgetary terms, tenable for the armaments industry, and therefore suitable as a whole for meeting future challenges. This in mind the briefing is presenting a comprehensive view and conclusions with regard to the conceptual design of CBRN defence within a multinational environment.
Tactical Medicine —°ICU capacities, structures and sustainability of German Armed Forces in missions abroad
Schmidbauer W, Veit C, Hölldobler G
Department of Anesthesiology and Intensive Care, Bundeswehr Hospital Hamburg, Germany
In the context of global missions Intensive Care medicine (ICU) is an elementary part of military medicine to treat severely injured or ill soldiers. Therefore all German medical facilities provide ICU capacities including complete respiratory and circulatory support as well as monitoring systems. The level of intensive care is adapted to European standards besides dialysis and hemofiltration. In role II facilities between 2 and 4 full equipped ICU beds are available, whereas field hospitals (role III) provide 4 – 8 ICU beds. ICU personnel consist of at least one ICU nurse per two ICU beds and one anesthesiologist. Length of ICU treatment should not exceed three days abroad to assure that in case of acute respiratory distress syndrome (ARDS) or acute renal failure patients can already be treated in a hospital in Germany. For both diseases a delayed onset of some days after trauma or injury is characteristic. Even if sustainability is not exactly defined because abroad ICU treatment has to be ensured all the time early medical evacuation to Europe helps to guarantee ICU sustainability. One challenge of tactical medicine is the management of mass casualty incidents (MCI) when resources, both personnel and equipment, are overwhelmed by the number and severity of casualties. Rapid extension of capacities, evaluation of all patients by triage, and acute treatment according to severity of trauma or disease are the most important items to manage MCI and to safe as many individuals as possible. Survival depends on the effective stabilization of vital function and on additional causal therapy. If biological or chemical weapons cause a MCI of poisoned or infected patients administering antidotes or antibiotics will be the needed casual therapy. In the case of MCI capacities of intensive care can be extended using portable emergency ventilators and monitors that are normally used as backup systems and on ambulances. This enables the facility at least to double ICU capacity. Oxygen should be produced by special generators to ensure nearly unlimited supply. Storage amount of drug including antidotes and antibiotics have to be calculated carefully and depends on the number of soldiers and the potential risk.
Limitations in Treatment of acute Chemical Warfare Agent Poisoning
Thiermann H, Worek F, Kehe K
Bundeswehr Institute for Pharmacology and Toxicology, Neuherbergstraße 11, 80937 Munich, Germany
Alleged use of chemical warfare agents in Syria made the headlines. Moreover, the motivation of terrorists today appears to be aimed at achieving maximal harm in the population. Thus, chemical warfare agents were shifted into the public focus. It appears that the most important threats arise from nerve agents and sulphur mustard. In case of an incident appropriate medical countermeasures must be available for a mass casualty scenario. At first, efforts have to be directed to ensure self-protection and protection of medical facilities from contamination. Exposure towards volatile nerve agents, e.g. sarin, results in fast development of cholinergic crisis. The clinical diagnosis should be confirmed as early as possible on-site by assessment of acetylcholinesterase activity. Unfortunately, treatment with autoinjectors that are filled with 2 mg atropine and an oxime (at present obidoxime, pralidoxime, TMB-4 or HI 6) is not effective against all types of nerve agents. Therefore, aggressive atropinisation should be considered already during the earliest stage of medical treatment. Oximes with a broad spectrum or a combination of different oximes as well as alternative strategies that enable survival in spite of high acetylcholine levels at synaptic sites should be developed. For the treatment of patients in whom ongoing cholinergic crisis has to be expected, e.g. after exposure to persistent nerve agents as VX, patient oriented treatment is necessary. In order to reduce the requirement of long-lasting artificial ventilation optimized oxime therapy according to the individual cholinesterase status should be performed. Strategies that are directed to reduce the poison load substantially in the patients should be developed. No specific antidote is available for sulphur mustard poisoning until now. Thus, treatment is directed to relieve harm by symptomatic measures as used for treatment of burns together with surgical or laser debridement. At any case, huge amounts of resources have to be expected to be consumed because wound healing is impaired. The therapeutic problem may aggravate due to possible depots of sulphur mustard in tissues. For substantially improvement of therapeutic options more basic knowledge on downstream signal pathway is necessary. An innovative and promising option consists in the use of stem cells.
Human adult stem cells under the influence of chemical warfare agents
Schmidt A, Thiermann H, Steinritz D
Bundeswehr Institute for Pharmacology and Toxicology, Munich, Germany
Introduction: The chemical warfare agent sulfur mustard (SM), also known as mustard gas, was first used in World War I. Although prohibited by the OPCW, significant amounts of SM still exist and have still to be regarded as a threat for military personnel and civilians. After SM exposure, the most prominent clinical symptom is the development of extensive non-healing skin wounds. This chronic wound healing dysfunction persists over long time. Mesenchymal stem cells (MSC) are known to play an important role in wound healing. Moreover, it is also known that patients with chronic wound healing diseases do have compromised mesenchymal stem cell functionality. Based on these observations and the known relationship between wound healing dysfunction and MSC function we investigated the impact of sulfur mustard on human MSC.
Material&Methods: Mesenchymal stem cells (MSC) were isolated from femoral head of healthy donors. They were cultured for not more then three passages. MSC were exposed with sulfur mustard in different concentrations. After exposure we analyzed apoptosis, cell survival, cell aging, migration ability and capacity of tissue specific differentiation.
Results: MSC demonstrated an unexpected high tolerance against toxic concentrations of SM, which is not evident in any other kind of cells. On the other hand a SM exposure (even at very low concentrations) showed negative effects on the migration capability as well as on MSC proliferation. An increase of apoptosis was not observed, whereas the cells demonstrated an accelerated senescence. Interestingly, the differentiation capacity was not significantly affected by sulfur mustard.
Discussion: The effect of sulfur mustard on MSC might play an important role in the persistence of long-term adverse effects. Moreover, our current results will help to understand the relationship between alkylating agents and MSC and thus will also give guidance in the future perspective for the therapeutic use of MSC in patients suffering from sulfur mustard induced chronic skin wounds.
Modified immunoslotblot assay to detect hemi and sulfur mustard DNA adducts
Kehe K, Schrettl V, Thiermann H, Steinritz D
Bundeswehr Institute of Pharmacology and Toxicology, Munich
Sulfur mustard (SM) is an old chemical warfare agent causing skin blisters (vesicant). Skin toxicity is thought to be partly caused by SM induced DNA damage. SM and the hemi mustard 2-chloroethyl ethylsulfide (CEES) are bi- and monofunctional DNA alkylating agents, respectively. Both chemicals react especially at the N7 position of guanine. The most abundant adducts are 7-hydroxyethylthioethylguanine for SM (61 %) and 7-ethyl thioethylguanin for CEES. Thus, DNA alkylation should serve as a biomarker of SM exposure. A specific monoclonal antibody (2F8) was previously developed to detect SM and CEES adducts at N7 position by means of immunoslotblot (ISB) technique (van der Schans et al. 2004). The aim of the presented work was to modify this protocol for use in a field laboratory. Briefly, human keratinocytes were exposed to SM and CEES (0-300 µM, 60 min). After exposure, cells were scraped and DNA was isolated and normalized. 1 µg DNA was transferred to a Nylon membrane using a slotblot technique. After incubation with 2F8 antibody, the DNA adducts were visualized with DAB staining. Blots were photographed and signal intensity was quantified. A staining was detectable in the range of 30 nM to 300 µM SM or CEES, respectively. However, DNA adducts were detected statistically significant after CEES and SM exposure above 30 µM which is even below the vesicant threshold concentration. Thus, the presented technique is potentially able to confirm SM or CEES exposure of patients exposed to low concentrations of these agents.
Therapy of nerve agent poisoning: Are new oximes promising?
Worek F, Wille T, Thiermann H
Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
Oxime-based acetylcholinesterase (AChE) reactivators are still the only causal therapy of poisoning by organophosphorus compounds (OP), i.e. nerve agents and pesticides. Clinically used oximes, e.g. obidoxime and pralidoxime, lack efficacy in case of poisoning by various nerve agents and pesticides and have limited ability to penetrate the blood-brain-barrier. These shortcomings resulted in the synthesis of an uncountable number of oximes in the past decades. Novel compounds are mostly tested in animal models and partially their ability to reactivate OP-inhibited AChE is investigated in vitro. Unfortunately, different in vitro and in vivo models are used by the various research groups which makes it hardly possible to compare the experimental data and to assess the potential therapeutic efficacy of novel oximes on a rational basis. Hence, we initiated an in vitro study to determine the reactivation kinetics of a large number of bispyridinium oximes with human AChE inhibited by structurally different OP. These experiments were undertaken under identical conditions in order to enable a direct comparison of the determined kinetic constants. The data gathered so far give insight into the impact of structural modifications on the affinity and reactivity of tested compounds. In addition, these results underline the difficulty to develop oxime-based reactivators having a broad spectrum against structurally diverse OP. The consequences of these findings will be discussed.
Receptor-active compounds as alternative approach for the treatment of nerve agent poisoning
Niessen KV, Seeger T, Thiermann H, Worek F
Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
The standard therapy of poisoning by organophosphorus compounds (OP) with atropine and oximes is of limited efficacy in case of different nerve agents and pesticides. This limitation initiated research efforts to provide novel approaches for an improved treatment. Hereby, bispyridinium non-oximes were tested in vitro and in vivo in different laboratories for their ability to improve OP-impaired neuromuscular transmission and to increase survival in combination with standard antidotes. The most promising compound was MB327, a bispyridinium compound with a propyl linker and tert-butyl groups at position 4 on both rings, which was synthetized by Dstl, Porton Down, UK. MB327 had a low affinity towards human and Torpedo californica nicotinic receptors and a moderate affinity towards human muscarine (M5) receptors. Soman-blocked neuromuscular transmission in human intercostal muscle and rat diaphragms could be restored significantly by MB327. Given as adjunct to physostigmine and hyoscine MB327 had a convincing therapeutic effect in soman, sarin and tabun poisoned guinea pigs. Hence, the bispyridinium non-oxime MB327 proved its therapeutic efficacy against highly toxic nerve agents in various in vitro and in vivo models and may be considered as a promising candidate for the further improvement of standard atropine and oxime therapy.
Cholinergic modulation of thiopental potency: A special case
Weimer I1,2, Seeger T2, Grasshoff C1, Thiermann H2, Antkowiak B1
1Department of Anaesthesiology and Intensive Care, Experimental Anesthesiology Section, Eberhard-Karls-University, Waldhoernlestraße 22, 72072 Tuebingen, Germany
2Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
Poisoning with organophosphorous compounds is associated with pathologically high concentrations of acetylcholine in the central and peripheral nervous system. If there is need for general anesthesia in intoxicated patients, the current literature suggests that the commonly used agents isoflurane, sevoflurane and etomidate might provide adequate anesthesia for performing surgical incisions only at high doses. However, due to their life-threatening side effects it is not a good option to supply these compounds in the high dose range. Thus it is an open question what anesthetics are indeed suited for treating such patients. In the present study we investigated the anesthetic efficacy of thiopental, making use of cultured organotypic slices derived from the mouse neocortex. This in vitro model has been validated previously by testing a considerable number of anesthetic agents. To determine the anesthetic efficacy of thiopental, action potential activity of cortical neurons was monitored in the presence and absence of the drug. Furthermore, the slice cultures were treated either with the nerve agent soman or with neostigmin, a reversible acetylcholine-esterase blocker. Acetylcholine was added at a concentration as typically observed during cholinergic crisis in vivo. To our surprise and in contrast to all agents investigated so far, excess of acetylcholine in the extracellular space did not decrease the efficacy of thiopental to reduce action potential activity of cortical neurons. These findings indicate that thiopental is capable to produce profound anesthesia in patients suffering from organophosphorous intoxication. Moreover, the concentration of thiopental required to provide adequate anesthesia seems to be largely independent on the degree of cholinergic overstimulation.
Organophosphate poisoning in the developed world - a single centre experience from here to the millennium
Hrabetz H1, Thiermann H2, Felgenhauer N1, Zilker T1, Haller B3,Eyer F1
1Department of Clinical Toxicology, II. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Ismaninger Str. 22, 81675 Munich, Germany
2Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
3Institute of Medical Statistics and Epidemiology, Klinikum rechts der Isar, Technische Universität München, Ismaningerstr. 22, 81675 Munich, Germany
Organophosphate (OP) poisoning still contributes to fairly high morbidity and mortality rates, both in resource-poor settings and in well-developed countries. Despite an impressible number of publications dealing with this particular poison, detailed clinical data on the more severe overdoses with these agents are relatively sparsely reported. A retrospective study was consequently conducted on 33 patients with OP poisoning admitted to our intensive care unit to provide additional data on clinical features. We included moderate to severe poisonings between 2000 —°2012 who required admission to ICU. Patients ingested dimethyl-OPs in 19 cases, diethyl-OPs in 8 cases and otherwise classified OPs in 6 cases. Death (5/33) occurred rather late and only one of these fatalities died during ongoing cholinergic crisis. Of the survivors (28/33), 71 % recovered fully while 29% showed predominantly neurological disabilities before being transferred to neurologic rehabilitation. Aspiration pneumonia predominated in 27/33 patients and one patient died in refractory ARDS. The intermediate syndrome occurs twice and cardiopulmonary resuscitation has to be performed in 6/33 patients. Fatalities showed a significantly higher Poison-severity-score, APACHE-II-score and SOFA-score compared to survivors and they showed significantly longer QTctime in the ECG, lower systolic blood pressure and heart rate, a lower pH and a higher base excess at admission. Patients with diethyl-OPs required intubation significantly earlier and showed lower and more sustained inhibited activity of the plasmacholinesterase at admission compared to patients ingesting dimethyl- OPs. Treatment with atropine and obidoxime was comparably between these groups and severity of poisoning, outcome, hemodynamics at admission, duration of mechanical ventilation and length of stay in the ICU did not significantly differ between the group of dimethyl- and diethyl-OPs. We conclude that the fatality rate in our patient cohort treated in a well-stuffed and equipped ICU of a developed country is similarly high to the rate seen in developing countries. It was obvious that patients die rather late when severe cholinergic crisis has mostly be overcome and death was therefore related to nonpoison specific complications.
ChE status: a novel device for on-site therapeutic monitoring of patients poisoned by organophosphorous compounds
Wille T, Thiermann H, Worek F
Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
In case of organophosphorus compound (OP) poisoning a serious decrease of acetylcholinesterase (AChE) and butyrylcholinesterase (BChE) activity can be detected. Thus, a CE certified mobile in vitro test system (modified Ellman assay) for the analysis of AChE and BChE activity in whole blood was developed for its deployment in the field by the German Armed Forces. However, additional on-site determination of the reactivatability of OP-inhibited AChE with oximes and of inhibitory activity in patient plasma (resembling residual OP in plasma) is mandatory for (oxime) therapy control. This prompted us to develop a more advanced device (ChE Status) allowing on-site measurement of the complete cholinesterase status consisting of erythrocyte AChE and plasma BChE activity, reactivatability of erythrocyte AChE with obidoxime ex vivo and inhibitory activity in patient plasma. The new on-site device is an important tool for the attending physician not having a specialized laboratory at hand to refine and control the oxime therapy of OP-poisoned patients. Advantages and drawbacks of the new on-site device will be discussed.
Role of hypoxia in skin cells after exposure to sulfur mustard*
Popp T1, Deppe J1, Steinritz D2, Schmidt A2, Ries C1
1Institute for Cardiovascular Prevention, Ludwig-Maximilians-University of Munich, Pettenkoferstr. 9b, 80336 Munich, Germany;
2Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
Exposure of the skin to sulfur mustard (SM) leads to tissue destruction and symptoms of delayed wound healing. The underlying pathophysiological mechanisms are poorly investigated and up to now there is no sufficient therapy available. Under physiological conditions, injuries of the skin cause a decline in tissue oxygen levels (hypoxia). In skin cells present in the affected area, low oxygen conterations result in the activation of a specific signaling pathway that is crucially regulated by the activity of hypoxia inducible factor 1 (HIF1. Under normoxic conditions (21 % O2), HIF1 is present in the cells in its hydroxylated form which is readily degraded by the proteasome. Under hypoxic conditions (< 5 % O2), HIF1 can not be hydroxylated by the corresponding hydroxylases and thus accumulates in the cytoplasm. This allows HIF1 to translocate into the nucleus and induce the expression of specific target genes which influence multiple cellular processes such as proliferation, migration, autophagy, and apoptosis that ultimately promote tissue repair and regeneration. According to our hypothesis, SM may interfere with HIF1 modulated processes in skin cells and thereby contributes to the impaired wound healing observed in SM-injured tissue. Our preliminary data indicate that exposure of primary keratinocytes and fibroblasts to SM affects HIF1 signaling in vitro as determined by cultivation of SM-treated and non-treated cells under hypoxic conditions (< 5 % O2). Moreover, contaminating the cells with SM alters the expression levels of factors important in the regulation of autophagy, a cellular process that is essential for cell survival under stress conditions. Further elucidation of molecular pathomechanisms contributing to SM-induced impairment in wound healing may improve the development of specific target-directed drugs for therapeutical intervention in SM-affected patients.
* Acknowledgement: This work was supported by contract with the German Federal Ministry of Defense (M/SABX/ 8A002).
Poly(ADP-Ribosyl)ation inhibitors as a pharmacologic approach to the therapy of sulfur mustard induced skin lesions*
Bürkle A
University of Konstanz Molecular Toxicology Group, Department of Biology, Konstanz, Germany
Sulfur mustard (2,2’-dichlorodiethylsulfide; SM) is a highly toxic and mutagenic warfare agent classified as a weapon of mass destruction. As soon as SM was first used as a warfare agent, research aimed at the development of an effective antidote. Early studies with first-generation inhibitors of poly(ADPribose) polymerases (PARP) have revealed promising therapeutic potential in SM-induced skin injury, but the underlying mechanisms remain elusive. The current renaissance of PARP inhibitors in cancer chemotherapy has revived the discussion on their treatment potential in SM pathology. We performed a comprehensive study to elucidate the role of poly(ADP-ribosyl)ation in SM-induced toxicology using SM and derivatives, such as nitrogen mustard (HN2) and 2- chloroethyl ethyl sulfide (CEES). Substance-specific DNA lesions were induced by CEES in a dose-dependent manner in living human keratinocytes (HaCaT) and these lesions were repaired after 24 —°48 h as evaluated by immuno-chemical methods. We observed that poly(ADP-ribose) formation is induced in HaCaT upon treatment with SM, HN2, and CEES, revealing substance-specific poly(ADP-ribosyl)ation dynamics. In order to elucidate the underlying molecular mechanism of PARP activation, we performed knockdown experiments of representative base excision and nucleotide excision repair proteins, such as APE1 and ERCC1, respectively. Whereas the reduction of APE1 expression had no effect on PARP activity, interestingly, the knockdown of ERCC1 almost completely abolished the CEES-induced cellular PAR production. These results indicate a functional involvement of poly(ADP-ribosyl)ation in the repair of CEES-induced DNA lesions. While our data indicate that PARP activity is not obligatory for the survival of cells upon CEES treatment, pharmacological inhibitor studies revealed that PARP inhibition sensitizes HaCaT cells for the induction of CEES-induced genomic instability, as evaluated by a micronuclei formation assay. In conclusion this study demonstrates that poly(ADP-ribosyl) - ation plays a functional role in mustard-induced toxicological mechanisms, which renders it an interesting therapeutical target in SM-related pathologies.
*Acknowledgement: This work is supported by the German Armed Forces Grant E/ UR3G/AG001/9A804
Human butyrylcholinesterase isolated from plasma for analytical method development
John H1, Breyer F2, Mizaikoff B2, Thiermann H1
1Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
2Institute of Analytical and Bioanalytical Chemistry, University of Ulm, Germany
Organophosphorus poisons (OP) like nerve agents or pesticides covalently bind to butyrylcholinesterase (hBChE, EC 3.1.1.8) thus inhibiting the hydrolyzing enzyme. Consequently, hBChE is thought to become an effective scavenger useful for therapeutic treatment of OP poisoning and its corresponding OP adducts are valuable biomarkers for analytical verification purposes [1]. Therefore, related research requires the pure endogenous human enzyme that unfortunately is not commercially available from respective suppliers in an appropriate quality. Accordingly, a modified procedure primarily based on the findings of Lockridge et al. [2] and Saxena et al. [3] was developed to purify the enzyme from human citrate plasma as natural source. hBChE was isolated from plasma by four consecutive chromatographic steps. In general, protein elution was monitored on-line by UV-detection (280 nm) and eluates of each purification step were fractionated continuously for off-line analysis of i) hBChE enzyme activity by Ellman assay, ii) protein purity by gel electrophoresis, and iii) protein identity by MALDI mass spectrometry and electronic MASCOT database search. Fractions of highest activity were subjected to the next chromatographic step, respectively. Initially plasma proteins were fractionated by two different polyethylene glycole 6000 (PEG 6000) concentrations yielding precipitated hBChE. Subsequently, the redissolved enzyme fraction was separated by anion exchange chromatography, affinity chromatography and two steps of size exclusion chromatography. During the entire purification process a number of separated protein impurities were identified exhibiting chromatographic properties similar to hBChE. Even though the entire yield of hBChE was quite low (3 % of the initial plasma amount) the high purity enabled studies to characterize glycosylation and enzyme activity.
References: [1] John H et al., In: Handbook of toxicology of Chemical Warfare Agents (R Gupta, ed.), Academic Press/Elsevier, Amsterdam (2009) 755-790. [2] Lockridge et al., J Med Chem Biol Radiol Def 3 (2005) 1-20. [3] Saxena et al., Protein Express Purif 61 (2008) 191-196.
Silibinin as a potential therapeutic for sulfur mustard injuries*
Balszuweit F, Schmidt A, John H, Kehe K, Thiermann H, Steinritz D
Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
Introduction: Sulfur mustard (SM) is a vesicating chemical warfare agent causing skin blistering, ulceration, impaired wound healing, prolonged hospitalisation and permanent lesions. Silibinin, the lead compound from Silybum marianum, approved for therapeutic use against Amanita phalloides (Green deathcap) poisoning, has also been discussed as a potential antidote to SM poisoning. However, its efficacy has been demonstrated only with regard to nitrogen mustards. Moreover, there are no data on the efficacy of the water-soluble prodrug silibinin- bis-succinat (silibinin-BS).
Aim: We investigated the effect of silibinin-BS treatment against SM toxicity in HaCaT cells with regard to potential reduction of necrosis, apoptosis and inflammation including dosedependency of any protective effects. We also aimed to demonstrate the biotransformation of the prodrug into free silibinin.
Methods: HaCaT cells were seeded in multi-well plates, exposed to SM (30, 100 and 300 µM) for 30 min and treated thereafter with silibinin-BS (10, 50 and 100 µM) for 24 hours. Necrosis and apoptosis were quantified using the ToxiLight BioAssay and the nucleosome ELISA (CDDE). Pro-inflammatory cytokines IL-6 and IL-8 were determined by ELISA. Ha- CaT cells, incubated with silibinin-BS were lysed and investigated by LC-MS/MS.
Results: LC-MS/MS results suggest that silibinin-BS is absorbed by HaCaT cells and biotransformed into free silibinin. Silibinin-BS dose-dependently reduced SM cytoxicity, even after 300 µM exposure. Doses of 50-100 µM silibinin-BS were required for significant protection. Apoptosis and interleukin production remained largely unchanged by 10 – 50 µM silibinin- BS but increased after 100 µM treatment.
Conclusion: Observed reductions of SM cytotoxicity by postexposure treatment with silibinin-BS suggest this as a promising approach for treatment of SM injuries. Whilst 100 µM silibinin- BS is most effective to reduce necrosis, 50 µM may be safer to avoid pro-inflammatory effects. Pro-apoptotic effects after high doses of silibinin-BS are in agreement with findings in literature and might even be useful to eliminate cells irreversibly damaged by SM. Further investigations will focus on the protective mechanism of silibinin and its prodrug and should establish an optimum concentration for treatment. The fact that the compound is already an approved therapeutic might facilitate its introduction into therapy of SM injuries, compared to the development of a completely new drug.
*This work has been accepted for publication in Chemico-Biological Interactions on June 17, 2013.
Participation in the Second Confidence Building Exercise on Biomedical Sample Analysis
Koller M
Bundeswehr Institute of Pharmacology and Toxicology, Munich, Germany
Since 2009, the Organisation for the Prohibition of Chemical Weapons (OPCW) is performing so-called Confidence Building Exercises to encourage laboratories all around the world to analyse biomedical samples for biomarkers of chemical warfare agents (CWA). February 2012, the samples for the second exercise were sent to the participating laboratories including Bundeswehr Institute of Pharmacology and Toxicology (IPTBw). On February 22nd, IPTBw received five urine samples numbered 201/07 – 205/07 where 07 was our laboratory code. The instructions by OPCW said that these urine samples were to analyse for metabolites of nerve agents (O-alkyl methylphosphonic acids, i.e. EMPA, IMPA, PMPA) and for metabolites of sulphur mustard (thiodiglycol, TDG, and ß-lyase products, SBMSE and MSMTESE) within the next 28 days. IPTBw performed the following methods: LC-MS/MS of O-alkyl methylphosphonic acids after SPE from urine, LC-MS/MS of TDG after SPE from urine, LC-MS/MS of SBMSE and MSMTESE after SPE from urine, and GC-MS of SBMTE obtained after reduction of SBMSE and MSMTESE in urine and final SPE from the reduction mixture. After all methods had successfully been applied to the five urine samples, IPTBw reported the results to OPCW on March 15th. Sample 201/07: SBMSE/SBMTE and TDG, sample 202/07: EMPA and PMPA, sample 203/07: IMPA, sample 204/07: IMPA and PMPA, and sample 205/07: SBMSE/SBMTE. The spiking protocol provided by OPCW on April 13th confirmed these results.
Poster
Novel Small Molecule Scavengers for Nerve Agents based on Bifunctional Hybrid Compounds*
Amitai G, Bar Ner N., Gez R, Chapman S, Elimelech DK, Ashkenazi N
Division of Medicinal Chemistry, IIBR, Ness Ziona, Israel
Bio-scavengers toward toxic organophosphorus (OP) chemical warfare nerve agents (CWNA) are based on either stoichiometric or catalytic enzymes e.g. butyrylcholinesterase (BChE) or paraoxonase1 (PON1), respectively. Although catalytic bioscavengers could be administered at lower doses than stoichiometric enzymes they may still cause immunogenic response. Further, enzyme macromolecules create an excessive payload by their large size (MW 40 – 80 KD) while scavenging OP molecules that are > 100 – 200-fold smaller (150 – 300 D). Therefore, we have embarked on designing new small molecules scavengers (SMS) that will rapidly detoxify OP nerve agents. SMS could be administered i.m. or p.o. and their pharmacokinetics may be tailored by suitable formulations. The molecular design of novel SMS was based on combining two functions in a single molecule: 1.Direct nucleophilic attack on OPs causing their degradation 2. Reactivation of OP-inhibited AChE in situ. The direct attack on OPs was achieved by substituted benzhydroxamic acid (BHA) and pyridinehydroxamic acid (PHA) derivatives. The HA moieties were coupled via linkers to pyridine oximes thus yielding hybrid bifunctional compounds displaying both detoxification and reactivation activities. So far 26 new compounds were synthesized 6 of which were bifunctional hybrids. All synthesized compounds were highly soluble and stable in aqueous solution. The new compounds were tested for their detoxification rate towards sarin, cyclosarin, soman and VX under physiological conditions (pH = 7.4, 37oC). The fastest SMS toward OP agents, protecting AChE from inhibition in vitro, were mono- di- and tri-methoxy BHA and some hybrids with t1/2 ~ 1 min (1 mM SMS and 1 µM OP). The hybrid compounds 2-PAM-(CH2)3-4-PHA, 2-PAM-Xylyl-4-PHA and 2-PAM-CH2- 4-BHA-displayed rapid detoxification as well as reactivation potency toward OP-AChE conjugates. The hybrid 2-PAM- (CH2)3-4-PHA displayed 10-fold faster kinetics than 2-PAM toward cyclosarin-inhibited AChE. Some hybrid compounds exhibited high decontamination efficacy (> 98%) toward cyclosarin and VX on pig-ear skin in vitro. We have started to evaluate the efficacy of some SMS toward CWNAs in vivo.
*Supported by DTRA US DoD contract HDTRA1-12-C-0008.
Pharmacokinetics of nerve agent therapies*
Armstrong S
Biomedical Sciences Department, Dstl, Porton Down, UK
The combination of atropine, Avizafone and HI-6 has demonstrated efficacy against acute nerve agent exposure in a number of species [1]. Likewise, human butyrylcholinesterase (huBChE) bioscavenger has also demonstrated efficacy [2]. Determining the pharmacokinetic (PK) profile of these medical countermeasures is essential for progression through development to enable extrapolation of efficacious doses and optimisation of dosing regimens. The PK of huBChE has been well-researched to determine its longevity following administration (desirable for proposed use as a pretreatment). In contrast, the PK profiles of the conventional medical countermeasures are not well understood in the guinea-pig, which is the proof-ofconcept small animal species of choice. To address this, PK profiles of atropine, diazepam and HI-6 were determined in the guinea pig, as was the profile of huBChE for comparison. Conventional medical countermeasures were administered individually by the intravenous route, via indwelling cannulae, or in combination by the intramuscular route ([atropine sulphate 5.8 mg/kg or 17.4 mg/kg, respectively], [avizafone hydrochloride 1.05 mg/kg or 3.14 mg/kg, respectively] and [HI-6 dimethanesulphonate 9.3 mg/kg or 27.9 mg/kg,respectively]). HuBChE (3.4 mg/kg) was administered by the intravenous or intramuscular routes. Blood samples were collected from animals and analytes were measured using LC-MS-MS. PK analysis was completed on the concentration-time profile data. Atropine, diazepam and HI-6 were rapidly absorbed, distributed and eliminated in the guinea pig with bioavailbilities being 0.99 ± 0.14, 0.53 ± 0.14 and 0.62 ± 0.27, respectively. In contrast, huBChE was slowly absorbed (intramuscular tmax 28 hours) and eliminated (intramuscular t½ 85 ± 13 hours), circulating in blood for at least 7 days following administration, in agreement with previously- published data. These PK studies, carried out for the first time in conscious, ambulatory guinea-pigs, provide data on the rapid clearance of conventional medical countermeasures in contrast to huBChE. These PK data can now be utilised in interpretation of medical countermeasure efficacy (see Combination Therapy for Percutaneous Nerve Agent Poisoning), to aid the design of future animal studies to optimise efficacy against nerve agent poisoning by different routes of exposure and for extrapolation of efficacious doses to the human situation.
* © Crown Copyright. Dstl 2013.
References: [1] Lundy PM, Hamilton M G, Sawyer TW, Mikler J: Comparative protective effects of HI-6 and MMB-4 against organophosphorous nerve agent poisoning. Toxicology 2011; 285 (3): 90-96. [2] Lenz DE, Clarkson ED, Schultz SM, Cerasoli DM: Butyrylcholinesterase as a therapeutic drug for protection against percutaneous VX. Chemico-Biological Interactions 2010; 187 (1-3): 249-252.
Possibilities of continual determination of cholinesterase activity in the rat blood in vitro and in vivo*
Bajgar J1,2, Kassa J1, Stetina R1, Cabal J1, Pavlik M1
1Department of Toxicology, Faculty of Military Health Sciences, University of Defence, Hradec Kralove;
2Department of Radiology and Toxicology, Faculty of Social and Health Studies, University of South Bohemia, Ceske Budejovice, Czech Republic
Trigger mechanism of nerve agent action is inhibition of cholinesterases, preferably acetylcholinesterase (AChE, EC 3.1.1.7) at the cholinergic synapses. Before its toxic action, the agent penetrates into the organism and, it is distributed to the target sites (peripheral and central nervous system) by a transport system (the blood). We developed the method of continual determination of blood cholinesterase activity allowing studies of different factors influencing the activity, e.g. the effects of nerve agents, reactivation of cholinesterases in the blood following administration of various oximes, the influence of prophylactics including horse butyrylcholinesterase etc. Generally, the groups of female Wistar rats weighing 250 – 270 g (n = 3 – 6) were premedicated (ketamine and xylazine) and cannulated to v. jugularis. Continual blood sampling (0.02 ml/min) and monitoring of the circulating blood cholinesterase activity were performed (the activity represents all enzymes hydrolyzing acetylthiocholine). Normal activity was monitored 1 – 2 min and then the agent (VX) was administered i.m. in dose of 2 x LD50. Using different routes of administration of the agents and antidotes at different time intervals before/following agents injection, cholinesterase activity was monitored and the changes in the activity were registered. The same procedure was applied in vitro when the blood was sampled from the animal and heparinized. Examples of some results are demonstrated. The results suggested that the method is suitable for comparison of the blood cholinesterase activity changes in vitro and in vivo.
* Acknowledgement: The study was supported by the grant of Ministry of Defence, „A long term organization development 1011“.
Choice of lyophilization conditions for the new auto injector with HI6 by the French forces
Bardot S, Besse Bardot I, Pech A
Pharmacie Centrale des Armées, Orleans, France
INEUROPE® is the french forces treatment against organo - phosphorus agents. It’s an authorized medicine including atropine, pralidoxime and avizafone. In 2010, French forces decided to replace pralidoxime by DMS HI6 and started the regulatory development of this new product. HI6 has a larger spectrum against organophosphorus agents. With the experience of INEUROPE manufacture, the “pharmacie centrale des armées” studied the lyophilization cycle for the new therapy. The lyophilization is a method of desiccation by sublimation of ice after freezing solutions. The parameters to choice the process of lyophilization are linked with the characteristics of the product in solution: cryoscopic fall, formation of eutectic elements, under cooling, temperature (full or partial freezing), homogeneity, speed of cooling, risk of insolubilisation. The development also has taken into consideration the stability and physical specifications of obtained product. These results of galenic development could allow providing “GMP manufactured” therapeutic unities in 2013 in order to collect clinical data necessary for the marketing authorization.
A compelling retrospective: Chemical structure of midazolam confers unique properties that make it a practical medical countermeasure for nerve agent-induced seizures
Belluscio BA, Shukla R
Meridian Medical Technologies, Inc, Columbia MD, USA
Midazolam contains an imidazole ring fused to the diazepine nucleus: a structure that confers three properties relevant to the practical aspects of clinical use (Gerecke, 1983). First, the ringopened state of the diazepine nucleus, which occurs due to hydrolysis at low pH, is stabilized by the basicity of the imidazole ring. In this state the molecule can exist in salt form, allowing formulation in aqueous solution and making intramuscular (IM) injections tolerable. Once injected, the physiological pH causes midazolam to revert to a ring-closed, highly lipophilic state with a t½ of 4 min (Loftsson, 2001), facilitating uptake from muscle. Following IM injection, the tmax of midazolam (< 30 min, Creviosier, 1981; Bell, 1991), is shorter than that of diazepam and avizafone (90 min and 45 min, respectively, Abbara, 2009). The lipophilicity also facilitates transit across the blood-brain barrier, with a t½ of 17 seconds and EEG effects within 30 seconds (Arendt, 1983). These pharmacokinetics may contribute to the finding that IM midazolam more rapidly terminates nerve agent-induced seizures in an animal model than many benzodiazepines, including lorazepam and avizafone (McDonough, 1999). Second, the methyl group on the imidazole ring is rapidly oxidized to an inactive form by liver enzymes, so that it has a relatively short duration of action (Gerecke, 1983). Following IM injection, the t½ is approximately 3 hours (Bell, 1991), also the time at which clinical effects abate (Crevoisier, 1981). Third, the imidazole ring provides for extended stability in aqueous solution. This is a critical characteristic for a substance that may be stored for long periods prior to use. Thus, due to its physiochemical properties, midazolam has rapid absorption and anticonvulsant effects when given IM, a short duration of action, and prolonged stability, making it a practical medical countermeasure for the treatment of nerve agent-induced seizures.
References: Abbara C et al., Br J Pharmacol 2009; 157(8): 1390- 1397.; Arendt RM et al., J Pharmacol Exp Ther. 1983; 227 (1): 98-106.; Bell DM et al., Epilepsy Res 1991; 10 (2-3): 183-90; Creviosier C et al., Drug Res 1981; 31(ii): 2211-2215; Gerecke M., Br J Clin Pharmacol. 1983; 16 Suppl 1: 11S-16S; Loftsson T et al., Int J Pharm., 2001 Jan 5;212 (1): 29-40; McDonough A et al., Archives of Toxicology 1999; 73: 473-478.
Pharmaceutical development for the new auto injector with HI6 by the French forces
Besse Bardot I, Bardot S, Pech A
Pharmacie Centrale des Armées, Orleans, France
After a first meeting with the French and German regulatory health authorities in 2010, the French military health service applied the development plan suggested for the new auto injector with HI6/atropine/avizafone in order to treat field organophosphorus neurotoxic intoxication. The pre clinical studies have been conducted in rat and cynomolgus monkey. The results allowed evaluating the safety to use the HI6 new molecule alone and in association. So, it is now possible to plan in 2013 the clinical trial in healthy volunteers. This project has been led in the scope of an arrangement between French and German countries. The target is to submit the marketing authorization documentation in both countries in 2015.
Micro-Nanoparticle Suspension Formulation Development for Medical Chemical Countermeasures*
Cabell L1, Clark A1, McDonough J1, Belski TT2, Mobley LR2
1Southwest Research Institute®, San Antonio, Texas, USA
2Chemical Biological Medical Systems, Medical Identification and Treatment Systems, Joint Product Management Office, Frederick, Maryland, USA
Current, U.S. medical chemical countermeasures require battlefield stability and an effective shelf life. One example is bispyridinium oximes that are used for the treatment of Organophosphate (OP) intoxication to counter the effects of AChE inhibition. This class of oximes possesses poor thermal stability in an aqueous formulation due to hydrolytic cleavage. CBMS and SwRI have developed non-Newtonian suspension formulations of oximes in cottonseed oil (CSO) vehicles that impart oxime solid stability characteristics to oxime/CSO liquid suspension formulations. MMB4 DMS and HI-6 DMS have shown superior thermal stability in these liquid suspension formulations compared to aqueous formulations and equal thermal stability compared to solid formulations. These types of formulations have shown bioavailability comparable to parent active pharmaceutical ingredients (API) in aqueous formulations. Cmax and Tmax for these APIs are relatively the same with absorption and elimination not substantially affected. In principle, these types of suspension formulations can be used to stabilize any drug that is prone to hydrolytic cleavage. In addition, the nature of these suspensions inhibits drug-drug interaction in the formulations as well as promotes differential drug controlled release if designed appropriately. We have designed these suspensions with high zero-shear viscosity, which allows it to resist sedimentation and non-Newtonian behavior that causes shear thinning, such that the viscosity decreases and the product flows easily under a shear force, such as injection through a needle. Furthermore, the viscosity and sedimentation behaviour are controlled by formulation parameters such as particle size and concentration.
* DISTRIBUTION STATEMENT, A. Approved for public release; distribution is unlimited.
A High Throughput Screen for Serine-198 Adducted Butyrylcholinesterase in Human Sera by Immunomagnetic Separation and HPLC-MS/MS Analysis
Carter MD1, Crow BS1; Pantazides BG2, Watson CM2, Blake T1, Johnson RC1
1Division of Laboratory Sciences, National Center for Environmental Health, Centers for Disease Control and Prevention, Atlanta, GA, USA;
2Oak Ridge Institute for Science and Education, Fellow at the Centers for Disease Control and Prevention, Atlanta, GA, USA
Human butyrylcholinesterase (HuBChE) enzymatic activity is used as a clinical measure of nervous system suppression by organophosphorus agents. The clinical measurement of HuBChE enzymatic activity, however, lacks the specificity of this immunomagnetic separation HPLC-MS/MS method. This high throughput screening method allows analysts to examine 100 sera samples/15 hours to confirm serine-198 BChE adduction, if present. Unlike previous methods which measure HuBChE enzymatic activity alone, this method allows analysts to confirm or exclude serine-198 adducts of BChE in human serum. This is a significant contribution since the variability of measured HuBChE enzymatic activity can range by 22 % (Nigg, H; et al. 2000) and would not be assumed a naturally “good” screening target (Zhang; et al. 1999). With a pooled QC serum Z’ score of 0.57 and a naturally lower individual sera Z score of 0.28, the assay is rated an “excellent assay” for the quality controls used and a “double assay” when used to screen patient samples. The assay is capable of distinguishing unadducted from adducted HuBChE with confidence. Hits, defined as samples with BChE Ser-198 adducts or no BChE present, are then analyzed in secondary and tertiary methods for identification and quantitation of the BChE adduct, if present. The ability to narrow the samples for additional analyses is of particular importance in a mass casualty. In an initial blind screen, 67 out of 70 samples were accurately identified giving a screen accuracy of 96 %. There were 42 known hits submitted for screening; the 42 hits were confirmed plus 3 false positives giving a high confirmation rate of 93 %. No false negatives were observed. Further optimization using flow injection reduces the screen’s instrument analysis time by approximately 90 % to 100 samples/1 hr. The method’s protocols are consistent with confirmatory analyses so that hits can be analyzed immediately following the screen. Due to the versatility of the screen target HuBChE, samples can be screened for the effects of a number of cholinesterase inhibitors and for a relatively low cost of $40 per well. This method is the first to provide a clinical and forensic high throughput screen for serine-198 adducted butyrylcholinesterase.
Addictive substances, drugs and metals – diagnosis using hair
Florek E, Kulza M, Wozniak A, Senczuk-Przybylowska M
Laboratory of Environmental Research, Department of Toxicology, Poznan University of Medical Sciences, Poznan, Poland
Hair, due to its unique properties, are considered to be an important source of information on exposure to xenobiotics. The history analysis dates back to the nineteenth century, when arsenic was indicated in the hair of exhumed corpses after 11 years. The next step in the analysis was to determine amphetamine in the hair of guinea-pig and determination of opioids using radio-immunological methods (RIA). However it was the introduction of GC-MS analysis which resulted in the growing popularity of hair analysis. This excluded the possibility of false positives (which took place in the immuno-enzymatic methods). Since then, there has been a rapid development of extraction methods of xenobiotics from the hair. It was used in the analysis of a number of substances, such as widely understood drugs of abuse (e.g. amphetamines, opiates, substances used in doping, pharmaceuticals, physiological and toxic metals). Knowledge about hair analysis developed very quickly and the results were used in some cases, such as lawsuits e.g. in the USA. The results of hair analysis for drugs have been used for the first time in court in 1982. This technique is used in order to confirm or exclude alcohol addiction. Hair analysis is also practically used in post-mortem toxicological studies and in relation to time away exposure (week-month-year). Segmental analysis of hair (hair cut into 1 – 2 cm pieces) provides information about the history of the adoption of addictive substances. The unique physiology and structure of the hair provides a number of ways of incorporating and elimination of xenobiotics. In the case of pregnant women one of the most common hazard to the fetus is tobacco smoke. The results of conducted studies indicate the possibility to measure the concentration of nicotine in the hair as a marker of long-term exposure to tobacco smoke. Extensive use of hair analysis is possible due to the development of modern and sensitive analytical methods. At present, analytical techniques such as GC-MS (gas chromatography combined with mass spectrometer), GC-MS/MS, LC-MS, LC-MS/MS become a powerful tool in the toxicological diagnosis for forensic purposes or in doping detection.
Comparison of Tandem and High-Resolution Mass Spectrometry for the Analysis of Nerve Agent Metabolites in Urine*
Hamelin EI1, Bragg W2, Shaner RL1, Swaim LL1, Johnson RC1
1Division of Laboratory Sciences, National Center for Environmental Health, Centers for Disease Control and Prevention, Atlanta, GA, USA,
2Oak Ridge Institute for Scientific Education, Oak Ridge, TN, USA
The use of a high-resolution accurate mass spectrometer (HRMS) was evaluated for the quantitation of nerve agent metabolites in urine. The results obtained using a mass resolution of 50,000 and a mass extraction window of 10 ppm around the theoretical m/z were used for quantitation of each metabolite. The precision, accuracy, linearity and sensitivity were compared with the current selected reaction mode triple quadrupole tandem mass spectrometry [1]. This study included five hydrolysis metabolites in urine, used to determine human exposure to VX, RVX, GB, GD, and GF nerve agents from 1 – 200 ng/mL. The application of HR-MS operating in full scan mode allows the detection of other similar compounds while simultaneously quantitating the known metabolites. This is particularly useful for the identification of exposure to nerve agents not currently included in this panel. Initial HRMS results indicated comparable precision and accuracy of standards and quality control samples to the tandem MS method.
Refererence: [1] Swaim Leigh L, Rudolph C Johnson, Yingtao Zhou, Chris Sandlin, John R Barr: J Analyt Toxicol 2008: 32: 775-777. *This work has been accepted for publication in Rapid Communications in Mass Spectrometry on May 5, 2013.
Biomarkers for sulfur mustard induced ocular injury
Horwitz V, Dachir S, Cohen M, Gutman H, Cohen L, Fishbine E, Gore A, Kadar T
Department of Pharmacology, Israel Institute for Biological Research, Ness Ziona.
The sight threatening sulfur mustard (SM) induced ocular injury presents specific clinical symptoms for each injury stage. While the partially healed acute phase is characterized by erosions and severe inflammation, the permanent delayed pathology that is developed only in part of the eyes, is clinically expressed by epithelial defects and neovascularization (NV). The mechanisms underlying this injury are still in research. Aiming to improve the therapeutic strategies, we focused on finding non-invasive biomarkers that point out towards the pathological processes during the injury. Rabbit eyes were exposed to SM vapor and a clinical follow-up, using slit lamp microscopy and pachymetry, was carried out up to 4 weeks. Tear fluid and corneal samples were collected at different time points for measurement of MMP-2 and MMP-9 activities by zymography and VEGF, IL-8, IL-6, TNFa and IL-1ß levels by ELISA. Typical SM-induced ocular injury developed, including a partially healed acute phase that followed by a delayed pathology in 50 – 80 % of the eyes. In the tear fluid, elevation in MMP-9 activity and IL-8 level was measured. While MMP-9 activity remained high throughout the follow-up period in all of the exposed eyes, IL-8 levels decreased with the healing of the acute clinical symptoms. Higher levels of IL-8 in tear fluid and increased thickness of the peripheral cornea preceded the clinical manifestation of corneal NV. Biomarkers in the tear fluid are a sensitive tool for monitoring pathological mechanisms during the dynamic course of the ocular injury. These biomarkers can rationalize novel therapeutic strategies and serve as a tool for treatment evaluation. Moreover, IL-8 level in the tear fluid and peripheral corneal thickness at the early stages of the injury may be indicative for the future injury outcome and the need for a preventive therapy.
Model alignment for improved evaluation of medical countermeasures against chemical warfare agents (CWA)
Tunemalm AK1, Thors L1, Johansson S1, Mikler J2, Joosen M3, van Helden H3
1CBRN Defence and Security, Swedish Defence Research Agency, Umea, Sweden
2Casualty Management Section, DRDC, Suffield, AB, Canada
3TNO Department of Chemical Toxicology, Rijswijk, The Netherlands
Among different national labs, various models are used for developing and testing medical countermeasures against CWA. An initiative between Canada, Sweden and The Netherlands is presented, in which the objective of the collaboration is to develop strategies and methods in order to obtain a shared base for the use of in vivo and in vitro models. Combined data from the three nations research efforts on pc VX exposure will be explored using multivariate data analysis tools such as Partial Least Squares in order to find correlations between the different models used today and to extract key information for prediction and future optimization of treatment of pc VX exposure. The immediate goal will be to collate and interpret data from each nation to explore the possibilities to provide a model to predict the outcome of the medical countermeasures and to improve the strategies regarding of a VX exposure to a human casualty. The long-term goal will focus on efforts to develop a model for translation of experimental with regard to skin penetration, including toxico-kinetics. Three different models, the in vitro epidermal skin penetration model, the hairless guinea pig and anesthetized swine, have been used to assess the characteristics of percutaneous VX absorption and to optimize the treatment regimens. To evaluate the window of opportunity for decontamination in these experimental set-ups, the Reactive Skin Decontaminant Lotion (RSDL) was used. The delay in absorption due to the skin barrier function presents a critical phase for decontamination and treatment but the amount of time is extremely variable. The depot of agent presents a continuous release of nerve agent which presents an additional challenge that needs to be addressed by a combination of effective decontamination and treatment. In conclusion, the ultimate aim is to develop a comprehensive research platform amongst the three partners that will provide, if successful, a more systematic approach regarding design of experiments and evaluation of results that cannot be achieved by the individual research programs. This would strengthen the outcome of each model, the comparison between models and allow for an extrapolation to human estimates.
A post-exposure therapeutic window to prevent the development of the delayed ocular injuries following sulfur mustard exposure*
Kadar T1, Horwitz V1, Amir A1, Cohen M1, Gutman H1, Sahar R1, Fishbine E1, Cohen L1, McNutt P2, Gore A1, Dachir S1
1Department of Pharmacology, Israel Institute for Biological Research, Ness Ziona, Israel
2USAMRICD Aberdeen Proving Ground, MD, USA.
Ocular injuries following sulfur mustard (SM) exposure are characterized by acute phase that may be followed by delayedonset irreversible corneal injuries that include epithelial defects, chronic inflammation and neovascularization leading to visual loss. Management of the late injury is complicated, therapy is symptomatic and only partially effective. Using our rabbit ocular model we defined the late injury as an ocular surface disease deriving from loss of corneal epithelial stem cells (SC), residing in the limbus (Limbal Stem Cell Deficiency, LSCD, Kadar et al., 2009). Although the precise mechanism underlying the death of the SC is not entirely clear, we have shown that the epithelial SC were not damaged primarily by SM but indirectly due to pathological processes in their niche that triggered the loss of SC later-on. Indeed, impairment of nerves and chronic inflammation were observed in the limbal stroma of eyes developing the delayed-onset injury (Kadar et al., 2011, 2012). The delayed death of the SC points towards the possibility of using a post-exposure prophylactic therapy, following the acute injury, to minimize the pathological processes in the SC niche and consequently to rescue the epithelial SC. Consistent with these findings, we have shown that administration of topical steroid (0.1% dexamethasone) or doxycycline, starting at one week following exposure, postponed the appearance and reduced significantly the incidence of the delayed lesions. The results confirm the presence of a post-exposure therapeutic window that can be used to prevent the development of the late ocular injuries. Further studies are required to evalute the effects of the treatments on corneal epithelial SC and their limbal niche.
*Acknowledgement: This work was supported in part by the Defence Threat Reduction Agency and, U.S. Army Medical Research and Material Command under Contract # W81XWH-08-2-0129.
References: 1. Kadar et al., (2009) Ocular injuries following sulfur mustard exposure – pathological mechanism and potential therapy. Toxicology 263:59-69. 2. Kadar et al., (2011) Delayed loss of corneal epithelial stem cells in a chemical injury model associated with limbal stem cell deficiency in rabbits. Curr Eye Res 2011;36:1098-1107. 3. Kadar et al., (2012) Prolonged impairment of corneal innervations after exposure to sulfur mustard and its relation to the development of delayed Limbal Stem Cell Deficiency. Cornea (Epub ahead of print).
The benefit of combinations of acetylcholinesterase reactivators for the antidotal treatment of poisoning with cyclosarin*
Kassa J1, Karasova JZ2, Stetina R1, Bajgar J1
1Department of Toxicology, Faculty of Military Health Sciences and
2Department of Public Health, Trebesska 1575, 500 01 Hradec Kralove, Czech Republic
The reactivating and therapeutic efficacy of two combinations of oximes (HI-6 + trimedoxime and HI-6 + K203) was compared with the effectiveness of antidotal treatment involving single oxime (HI-6, trimedoxime, K203) using in vivo methods. In vivo determined percentage of reactivation of cyclosarin-inhibited blood and tissue acetylcholinesterase in poisoned rats showed that the reactivating efficacy of both combinations of oximes is slightly higher than the reactivating efficacy of the most effective individual oxime in blood, diaphragm as well as in brain. Moreover, both combinations of oximes were found to be slightly more efficacious in the reduction of acute lethal toxic effects in cyclosarin-poisoned mice than the antidotal treatment involving single oxime. Based on the obtained data, we can conclude that the antidotal treatment involving chosen combinations of oximes brings a beneficial effect for its ability to counteract the acute poisoning with cyclosarin.
* Acknowledgement: The study was supported by the grant of the Ministry of Defense, Long-term organization development plan 1011.
Respiratory Toxicity in the Pig Model Following Sarin Exposure - Functions, Dynamics, Imaging and Arterial Blood Gas Analysis*
Katalan S
Division of Medicinal Chemistry, Israel Institute for Biological Research, Ness-Ziona, Israel.
Introduction: Exposure to sarin, a highly toxic cholinesterase inhibitor, induces an array of toxic effects and death if not treated. It is commonly accepted that respiratory failure is the leading cause of death following severe sarin intoxication, however the nature of Chemical Warfare Nerve Agents (CWNAs)-induced respiratory toxicity is not yet well defined.
Methods: Respiratory dynamics were monitored by wholebody barometric plethysmography prior and post exposing pigs to lethal (60 µg/kg; sc) and sub-lethal (37 µg/kg; sc) doses of sarin. In animals which were exposed to lethal dose of sarin (60 µg/kg; sc), arterial blood gases and chest X-ray (CXR) were taken and analyzed as well.
Results: All animals suffered from imminent respiratory distress showing a dose dependant response following sarin exposure. While the respiratory distress in the lethal dose group evolved to severe respiratory failure including hypoventilation, hypoxemia, acidemia and hypercapnia with no evidence of lung pathology on CXR, the animals in the sub-lethal dose group recuperated by exhibiting a notable compensating response of hyperventilation and tachypnea.
Discussion: Our work indicates that even after exposure to sublethal dose of sarin, the respiratory system is severely affected. After exposure to sub-lethal dose of sarin the deterioration towards terminal respiratory failure is avoided by endogenous spontaneous physiological processes which are mediated by the respiratory center. However, this compensating response is depressed after exposure to lethal dose of sarin. Thus, it is suggested that exogenous assisted mechanical ventilation expects to improve survival by overcoming the imminent respiratory depression which is ensued after exposure to deadly doses of CWNAs.
* Acknowledgement: The author would like to thank Amir Rosner, Shlomi Baranes and Inbal Egoz for their outstanding assistance, and to thank Eugenia Bloch-Shilderman, Yishai Karton and Zvi Teitelbaum for their helpful advice and support in this project.
Datum: 16.08.2013
Quelle: Wehrmedizinische Monatsschrift 2013/7